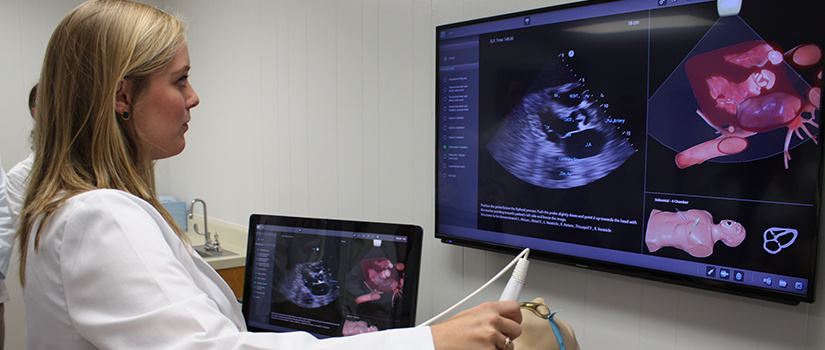
Point of Care Ultrasound
In 2006, we became the first university in the country to integrate ultrasound technology throughout a four-year medical curriculum. Since then, we've worked with our partners to create curricula, test new technologies and encourage medical providers around the world to use ultrasound technology in ways that improve the quality of patient care. We believe ultrasound should be a core competency because there are practical applications in almost all medical disciplines.
Back to the Bedside
The best place to teach the art, science and humanity of medicine is at the bedside. One of the benefits of ultrasound is that it provides you the opportunity to visit patients, to learn to talk to them and use the images as a teaching tool to help them understand their health.
Integrated Ultrasound Curriculum
You’ll be exposed to ultrasound technology throughout your curriculum. The focus will be on the applications most relevant to specific courses, clerkships, and electives.