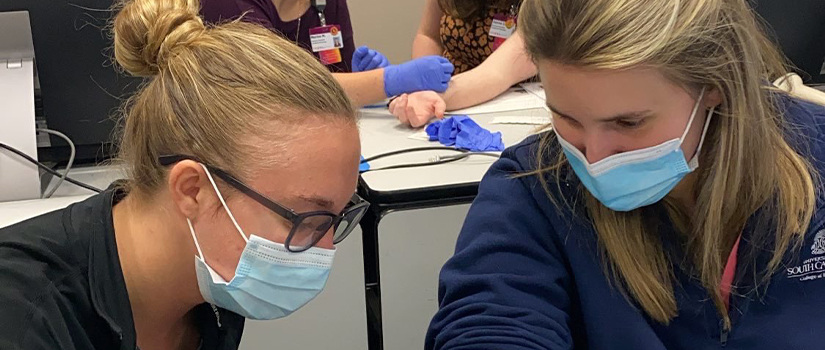
About the Program
While approximately 35 million Americans carry a penicillin allergy label, nearly 90% do not have a true allergy. Having a documented penicillin allergy leads to more negative health care outcomes including higher rates of adverse drug events, greater infection risks with resistant organisms, and higher overall health care costs. Our Penicillin Allergy Assessment and Skin Testing Certificate (PAAST) program is designed to hone skills of health care providers in allergy assessment and penicillin skin testing for the purpose of improving antibiotic selection and patient outcomes following allergy reconciliation.
At the conclusion, all participants completing the online material and live program portions will receive an official certificate documenting their competency. Whether you’re a trainee or seasoned practitioner, any health care provider involved in antibiotic administration, prescribing, and/or decision-making including nurses, pharmacists, nurse practitioners, physician assistants, and physicians, you'll find value in this program.
This 15-hour continuing education accredited program combines interactive and in-depth home study with live programming offered at host sites across the country.
The University of South Carolina is accredited by the Accreditation Council for Pharmacy Education as a provider of continuing pharmacy education. This is a practice-based activity which is accredited for a total of 15 contact hours (1.5 CEUs) for pharmacists (UAN 0062-9999-19-002-B01-P). Initial release date: January 5, 2019; expiration date: January 5, 2022. In order to complete this practice-based program, all pharmacists are required to view all home study modules in their entirety (participating in active learning components as prompted), pass the home study post-test (prior to attending the live session), and attend a live session in its entirety. No partial credit will be awarded. Credit will not be awarded for completing only the home study modules if a live session is not attended, and credit will not be awarded for completing only the live session if the home study modules are not completed and the post-test is not passed. In order to have credit reported to the NABP CPE Monitor, participants must complete the online program evaluations within 30 days of the live activity and must provide their correct NABP e-profile number and day/month of birth. Any credit claimed greater than 60 days from the date of the live activity will be automatically rejected by the NABP CPE Monitor.
Accreditation Statement:
This activity has been planned and implemented in accordance with the accreditation
requirements and policies of the Accreditation Council for Continuing Medical Education
(ACCME) through the joint providership of the Medical University of South Carolina
and the University of South Carolina College of Pharmacy. The Medical University of
South Carolina is accredited by the ACCME to provide continuing medical education
for physicians
Credit Designation
The Medical University of South Carolina designates the live activity for a maximum
of 4 AMA PRA Category 1 Credit(s)™. The Medical University of South Carolina designates the enduring activity for a maximum
of 11 AMA PRA Category 1 Credit(s)™ Physicians should claim only the credit commensurate with the extent of their participation
in the activity.
Mid-Carolina AHEC, Inc. is an approved provider of continuing nursing education by the South Carolina Nurse Association, an accredited approver with distinction, by the American Nurses Credentialing Center’s Commission on Accreditation. This nursing continuing education activity approval #1811-032PR-011 has been approved for 15.0 hours.
At the conclusion of the program, the participant will be able to:
- Evaluate antibiotic-associated allergies and the negative outcomes associated with documented beta-lactam allergies.
- Recommend appropriate first- and second-line therapies for common disease states that include beta-lactam antibiotics as a preferred therapy.
- Describe methods for successfully and safely optimizing antibiotic therapy in a patient with a documented penicillin allergy.
- Perform a comprehensive allergy assessment and assess the need for penicillin skin testing.
- Execute and interpret the results a penicillin allergy skin test.
- Implement a comprehensive allergy assessment and skin testing program at your institution.
Our program Advisory Board members and content authors are among the nation’s leading physician and pharmacist experts and scholars in penicillin allergy related outcomes and execution of comprehensive allergy assessment and skin testing:
- Christopher M. Bland, Pharm.D.
- P. Brandon Bookstaver, Pharm.D.
- Justin Chen, M.D.
- Nicole Griffith, Pharm.D.
- Emily Heil, Pharm.D.
- Bruce Jones, Pharm.D.
- Caitlin Mardis, Pharm.D.
- Nathon Parker, Pharm.D.
- Hana Winders, Pharm.D.
- Mary Staicu, Pharm.D.
- Nicholas Torney, Pharm.D.
- Luis Tulloch, MD
- Geoffrey Wall, Pharm.D.
November 27, 2018

The USC Student Society of Heath-System Pharmacy (SSHP) chapter created an educational task force to inform the community about penicillin allergies. Their first event was Saturday, November 3, at Soda City Market on Main Street in Downtown Columbia. The task force, accompanied by professors Julie Ann Justo and Hana Rac, set out to ask a simple question, “Are You Truly Allergic to Penicillin?” Seventy-one market attendees approached the booth to find out the answer.
Many of the booth visitors had questions about their own penicillin allergy or an allergy of a family member or friend. After task force members inquired when and how the reactions presented, a common theme from the public included reactions that occurred at a young age with nonspecific rashes, or stomach upset. Visitors to our booth were surprised to learn that after 10 years, even with a true allergy, up to 80% of patients lose their sensitivity. The task force also clarified the difference between drug side effects and allergic reactions.
During their time at the market the task force, with the help of Professors Justo and Rac, de-labeled two penicillin allergies. A ten-year old girl and her mother came to the booth to inquire about the girl’s allergy. She was labeled penicillin allergic at the age of 5 when she had a nonspecific reaction believed to be caused by the drug. The task force began to ask about her medication history. Her mom remembered many of the antibiotics the girl had taken over her lifetime including Omnicef and Rocephin - cephalosporin antibiotics which have similar structures to penicillin and a small chance of allergic cross-reactivity. At the end of the conversation, the mom briefly mentioned that the girl had also taken and tolerated Augmentin, which is a combination drug of amoxicillin and clavulanic acid. Additionally, a college-aged boy was de-labeled at our event after a brief investigation into his medication history based on his use and tolerance of amoxicillin in the past. Commonly, patients do not realize that amoxicillin is a penicillin antibiotic. If a patient who is labeled as penicillin allergic can tolerate amoxicillin, then they are no longer allergic to penicillin. With the right questions, pharmacists can remove their patients’ penicillin allergic labels allowing the use of more effective therapy and decreasing antibiotic resistance.
Furthermore, the task force excitedly discussed the penicillin allergy skin test and the role that pharmacists can play. It is currently available in select hospitals and clinics within South Carolina, with pharmacists administering the test in some of these settings. Many people were curious to hear about this one-hour test to determine true allergies that consists of a two-step process, including scratch testing and intradermal testing.
The SSHP penicillin allergy educational task force enjoyed helping the community investigate their penicillin allergies and can’t wait to continue educating Columbia residents at upcoming events.
September 26, 2018
We often say the Doctor of Pharmacy degree (Pharm.D.) is the most versatile degree in health care. Pharmacist roles continue to expand in many areas, especially in direct patient care. One such area is antibiotic stewardship. We are all called to be good stewards of our resources, and antibiotics are no exception. In general, antibiotic stewardship involves a multidisciplinary team working to optimize antibiotic selection, dose and duration based upon best available evidence. One challenge to effective antibiotic stewardship is the presence of antibiotic allergies, particularly a documented allergy to penicillin.
Nearly 10% of Americans have a penicillin allergy documented in their medical records. While up to 90% of these allergies are either not severe or altogether inaccurate, they can certainly complicate antibiotic decision-making. Pharmacists in South Carolina are working to change that paradigm. In the summer of 2016, the Board of Pharmacy, Nursing and Medical Examiners, through a joint Healthcare Consortium committee, approved a pilot program at Prisma Health Richland for pharmacist-administered penicillin allergy skin testing. Patients hospitalized at Prisma Health with a penicillin allergy who were evaluated by the Infectious Diseases Team or Prisma Health Antimicrobial Stewardship and Support Team (PHASST) were eligible for testing.
“To date, we have performed approximately 40 skin tests and have screened over 125 additional patients. The results have been remarkable and led to favorable antibiotic changes in nearly 80% of patients tested,” said Julie Ann Justo, Clinical Assistant Professor at the USC College of Pharmacy and Infectious Diseases pharmacist at Prisma Health. Justo went on to add that often a thorough investigation of the allergy by a pharmacist is enough to help optimize antibiotic decision-making. “The patients really appreciate knowing the status of their allergy and whether they can take penicillin or related antibiotics,” stated Justo. Full results of this pilot project will be presented by Class of 2019 USC COP student, Nicole Griffith, at the American College of Clinical Pharmacy Global Meeting in Seattle, Washington in late October.
Majdi Al-Hasan, M.D., medical director of PHASST and professor at the USC School of Medicine Columbia, recognizes the benefit. “Antibiotic stewardship is all about optimizing patient care. Our physicians and pharmacists at Prisma Health and USC are doing all they can to be good stewards of antibiotics in the era of increasing antibiotic resistance. Penicillin skin testing is one more tool we now have to ensure patients receive first-line therapy for serious infections.”
The Board of Pharmacy has since lifted the pilot restrictions and pharmacist-driven penicillin allergy skin testing is now approved throughout South Carolina, subject to appropriate credentialing, training and institution protocols and approval. Plans at Prisma Health include expansion into outpatient clinics and orthopedic surgery areas. A national certificate program for penicillin allergy assessment and skin testing available for pharmacists, physicians, physician assistants, nurses and associated trainees has recently been launched.
September 28, 2018
Penicillin allergies are quite common with over 30 million Americans and nearly 500,000 South Carolinians reporting an allergy to penicillin or related antibiotics. Penicillin, an antibiotic that has been on the market since the 1940s, is not as commonly used as it once was, but many other commonly prescribed antibiotics are related.
“Recognition of the accuracy of a true penicillin allergy is important,” said Brandon Bookstaver, Associate Professor at the USC College of Pharmacy and infectious diseases pharmacist at Prisma Health. Recent published medical literature has demonstrated that patients with documented penicillin allergies are at higher risk for infections after surgery and often receive costlier or potentially less effective alternative antibiotics. It offers the question, ‘what can be done’?
“It’s a combination of patient and provider education with detailed investigative work to get the true nature of the documented allergy” commented Hana Rac, the infectious diseases pharmacist for the Antimicrobial Stewardship Collaborative of South Carolina (ASC-SC) and clinical instructor at the USC College of Pharmacy. “If there is suspicion that there may be a true allergy, there are other ways to determine the accuracy, including a penicillin skin test,” Rac added. USC College of Pharmacy students and faculty have implemented pharmacist-driven penicillin skin testing at Prisma Health Richland, helping to improve detection of true allergies and optimizing antibiotic selection in these patients. Approximately 90% of patients with a documented penicillin allergy, in fact, do not have a true, serious allergy which can be determined through reconciliation and penicillin skin testing.
Penicillin allergy day reminds us the importance of good documentation of all drug allergies and the value in good detective work to determine if related medications can be prescribed safely. Bookstaver added, “Governor McMaster recognizes its value by declaring September 28 as penicillin allergy day in our state.” South Carolina is one of four states with an official proclamation of National Penicillin Allergy Day for 2018.
This program is supported by a generous unrestricted educational grant from ALK-Abello, Inc.